It is estimated that 5 million women in the US suffer from endometriosis. The numbers could actually be higher, but considering the nature of the disorder, it is frequently misdiagnosed. Some women wait years for an accurate diagnosis.
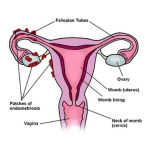
Endometriosis is a disease caused by the abnormal growth of the endometrium outside the uterus. The endometrium is the lining of the uterus. When it grows on the fallopian tubes, ovaries, along the pelvis or even on the colon, it can cause debilitating symptoms. During the regular menstrual cycles, the lining breaks down. In patients with endometriosis, it has nowhere to go. This can lead to cysts, heavy periods, severe cramps during and outside the menstruation and in some cases, infertility. The condition is a painful one, and it can remain undiagnosed for years.
Sometimes, women with endometriosis can lack the specific symptoms completely, which makes the real number of sufferers much higher. Severe cases of endometriosis can cause the lining of the uterus to grow in other parts of the body like the brain or lungs.
Causes
The exact causes of endometriosis are unknown. There are some frequent theories regarding the appearance and evolution of the condition.
- One of the most frequent theory is that during menstruation, blood mixed with endometrial cells flows back into the fallopian tubes. The cells install on different organs and start to grow outside the uterus.
- A second theory widely-popular with specialists is that endometrial cells are carried through the bloodstream to different parts of the body.
- Immune system disorders contribute to the development of the condition, according to another theory. When the immune system doesn’t properly detect and eliminate endometrial cells from outside the uterus, they install and spread in different areas of the body.
- The genetic factor is also floated as one of the causes of endometriosis. The condition can sometimes run in families.
Still, the medical world hasn’t discovered the exact causes that lead to endometriosis.

Symptoms
One of the most common symptoms in women with endometriosis is cramping during menstruation. In time, the cramping can worsen and become debilitating. Scar tissue formation is another cause of severe pain in women struggling with the condition. Scar tissue formation in areas where it doesn’t belong, like the fallopian tubes, bowels, brain or lungs can lead to further medical issues.
Although cramping during menstruation is normal in all women, the intensity is severe and debilitating, in women with endometriosis. It also amplifies over time. All women who experience pelvic pain should visit their gynecologist, especially if the pain is present long before their menstruation, at the beginning of the ovulation. Pain during intercourse, frequent urination, fatigue, and gastrointestinal problems are also common symptoms of the condition.
One of the ways most women with the condition find out about it is when they visit a medical practitioner for infertility issues or bleeding between periods.
Diagnosis
The only way to get a certain diagnosis is through laparoscopy. The intervention is a minor surgery where the doctor inserts a thin scope into the abdomen to analyze pelvic organs and remove endometrial tissue. In some cases, the specialist might want to perform a series of other tests, the head gynecologist at Emu Health says. Usually, doctors will perform a pelvic exam, together with an abdominal or vaginal ultrasound. While these tests cannot identify endometriosis, they can outline other conditions related to it, like cysts and fibromas. These tests are also performed to exclude other causes of the patient’s symptoms.
Treatment
There is no definitive treatment for endometriosis. However, hormonal treatment and painkillers, together with laparoscopy tissue removal will be performed. Hormonal treatment for women who want to get pregnant consists of gonadotropin-releasing hormone (GnRH) agonist. The hormone stops ovulation and is only prescribed for six months at a time. Pregnancy can occur only after the treatment stops.
Laparoscopy and laparotomy are common interventions used to treat endometriosis. However, the condition will return within two years.

Dietary Changes for Endometriosis Management
According to several studies, eating a healthy diet might stop the development of the condition. A 2013 study showed that women who ate more vegetables, fruits and omega-3 fatty acids were less likely to experience the usual symptoms. On the other hand, women who ate trans fats, red meat and drank large amounts of coffee were more likely to develop endometriosis. While not all studies offer consistent proof in favor of dietary changes, anecdotal proof shows that it’s possible to prevent the condition’s development through a diet consisting of:
- Vegetables;
- Fruits;
- Omega-3 fatty acids;
- Whole grains;
- Unprocessed foods.
While endometriosis cannot be prevented, eating the types of foods mentioned above might help. Avoiding foods that increase estrogen levels like caffeine and alcohol will help decrease the intensity of the symptoms.
Diet for Endometriosis
Women with endometriosis should consider a diet that prevents and reduces inflammation and estrogen level spikes. Healthy fats, fruits, and vegetables, as well as unprocessed foods, seem to help with decreasing the symptoms. Healthy fats can be found in the following foods:
- Olive oil;
- Olives;
- Avocados;
- Salmon;
- Nuts
- Fatty fish.
A gluten-free diet seems to also help reduce endometriosis symptoms. A 2012 study suggested that almost 80% of the women who partake in the study reported a decrease in their symptoms after they adopted a gluten-free diet. FODMAP diets have also become popular among women with the condition. It involves eliminating certain carbs and irritating foods from the diet. Endometriosis is causing severe gastrointestinal problems, and the main goal of this particular diet is allowing the intestine to heal and recover. After complete elimination of irritating foods, a person can start reintroducing them, to see which ones cause worse symptoms.
While dietary changes are absolutely necessary to lower the discomfort caused by the condition, frequent visits to your gynecologist are also important. Supervising the condition’s evolution and making adjustments to your hormone and painkiller prescription, in accordance with your condition’s evolution, is important for better general health.